Safety
Raw Milk Is Not a High-Risk Food
Industry and medical groups have claimed that raw milk is dangerous, but the data contradicts their claims.
Any food can be the source of foodborne illness under the wrong conditions. The issue isn’t whether some people have become sick from raw milk on occasion – the issue is whether raw milk poses such an unusually high level of risk that it justifies the government forcing people to drive several hours to the farm to obtain it.
All of the data discussed below is from the CDC for the 13-year period from 1998 to 2010.
Texas data on foodborne illnesses:
In Texas, between 1998 and 2010, only two people contracted foodborne illness attributed to raw milk. Neither was hospitalized, indicating relatively minor illness.
In the same time period, there were approximately 12,500 foodborne illnesses reported in Texas, not including people who became ill as part of multi-state outbreaks such as with spinach or peanut butter. Consider the illnesses attributed to other foods in Texas:
- Raw oysters: 486 illnesses and 20 hospitalizations
- Turkey: 852 illnesses
- Ham salad: 225 illnesses
In April 2011, the Texas Department of State Health Services (DSHS) announced that it had linked four illnesses to a raw dairy. The investigation is not complete and the details have not been released. If proven, it would mean that a total of six illnesses have been attributed to raw milk in the last 20 years in Texas (See testimony of DSHS at Public Health Committee hearing, 4/20/2011). More illnesses have been attributed to foods such as strawberries and chicken soup than to raw milk in Texas.
National data on foodborne illnesses:
Nationwide, there were 1,414 illnesses, 80 hospitalizations, and 0 deaths attributed to raw milk between 1998 and 2010. The CDC does not indicate how many of these illnesses were attributed to raw milk that came from dairies that were not licensed to sell raw milk to consumers. Dairies that are producing milk intended for pasteurization are not held to the same standards as Grade A Raw for Retail dairies, yet consumers often buy milk from these conventional dairies illegally. This “pre-pasteurization milk” poses a higher risk, as shown by the significantly higher incidence of positive pathogen tests from their bulk tanks. Thus, these numbers significantly overestimate the risk posed by raw milk from licensed, regulated dairies.
To put these numbers in context, there were 301,076 illnesses, 10,317 hospitalizations, and 223 deaths reported to the CDC in that time period from all foods. (See wwwn.cdc.gov/foodborneoutbreaks) Consider the illnesses attributed to other foods:
- Fruit salad: 1,323 illnesses, 29 hospitalizations, and 1 death
- Tuna: 1,355 illnesses, 36 hospitalizations, and 3 deaths (not including raw tuna or sushi)
- Deli meats: 1,345 illnesses, 104 hospitalizations, and 19 deaths
- Pizza: 1,614 illnesses, 20 hospitalizations, and 3 deaths
The numbers of illnesses attributed to fruit salad, tuna, pizza, and deli meat are similar to those attributed to raw milk during this time period – with the exception that, unlike these foods, raw milk has not caused any deaths. (Note: the numbers for deli meats do not include sandwiches, which have caused many more illnesses.) While more people may consume these foods occasionally, few people consume these foods day-in and day-out, in contrast to raw milk.
Consumption rates:
How many people drink raw milk? According to a CDC survey, an average of 3% of the population has drunk raw milk within the last 7 days. (Tab 2 – chart of raw milk consumption.) That translates to more than 9 million raw milk consumers. So, out of 9+ million consumers, approximately 112 become sick each year allegedly from raw milk nationwide, or 0.001%.
In Texas, a 3% consumption rate would mean that approximately three quarters of a million Texans drink raw milk, yet only two people have been reported ill from raw milk over a period of 11 years.
Chart Notes/References:
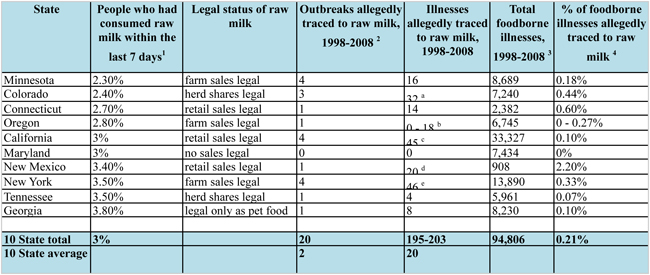
2 Note: an “outbreak” according to the CDC can involve as few as 2 people.
a In the same time period in Colorado, there was an outbreak linked to pasteurized milk that sickened 200 people
b Oregon was part of a multistate outbreak allegedly traced to raw milk in Nov. 2005. The total number of illnesses in that outbreak were 18, but we cannot determine how many occurred in Oregon.
c In the same time period in California, there were two outbreaks linked to pasteurized milk that sickened 1,744 people.
d The New Mexico illnesses are from a single outbreak listed as being from “1% milk, unpasteurized; sauces, unspecified” in a restaurant.
e In the same time period in New York, there were two outbreaks involving pasteurized milk that sickened 18 people.
3 The total foodborne illnesses are actually higher than listed in this chart because all data attributed to multi-state outbreaks was excluded for these purposes because the CDC table does not indicate how many illnesses were attributed to each state.
4 Because of the undercounting of the total number of foodborne illnesses (see note 2), the true % of illnesses allegedly traced to raw milk is lower than indicated.
Pasteurized milk also carries some risk of foodborne illness:
In the same time period, according to the CDC data, 2,227 people became ill, 27 people were hospitalized, and 3 died from pasteurized milk. A large number of people drink pasteurized milk, so the relative risk is not high, but pasteurization does not eliminate all risk.
In fact, a massive foodborne illness outbreak was linked to pasteurized milk in the 1980s. In 1985, there were over 16,000 confirmed cases of Salmonella infection that were traced back to pasteurized milk from a single dairy. Two surveys estimated that the actual number of people who became ill in that outbreak were over 168,000, “making this the largest outbreak of salmonellosis ever identified in the United States.” Ryan, CA et al. Massive outbreak of antimicrobial-resistant salmonellosis traced to pasteurized milk. J. American Medical Assn. 258(22):3269-74 (1987), www.ncbi.nlm.nih.gov/pubmed/3316720?dopt=Abstract
The 2013 Texas state bill (HB 46) would not allow the sale of soft, fresh raw cheeses, which pose a higher risk:
Some industry groups have presented higher numbers of illnesses allegedly due to raw milk, including two deaths. But these numbers are not attributable to raw milk, but rather to all raw dairy products. This is an important distinction because of the extensive problems reported from soft fresh cheeses such as raw queso fresco, which is illegal to sell but often imported from Mexico or made under unsanitary conditions at home and therefore nicknamed “bathtub cheese.” (See Queso Fresco: Cheese with a reputation.) Many of the illnesses and all of the deaths that the industry attributes to raw milk were in fact linked to raw queso fresco. HB 46 would not legalize the sale of soft, fresh raw milk cheeses such as queso fresco.
The data, as opposed to the rhetoric, shows that raw milk does not pose an unusually high risk of foodborne illness.
References:
- CDC data on foodborne illnesses, drawn from wwwn.cdc.gov/foodborneoutbreaks
- “Queso Fresco: Cheese with a Reputation,” Food Safety News, www.foodsafetynews.com/2010/05/queso-fresco-cheese-with-a-reputation